When Is Excisional Debridement Necessary for Chronic Wounds?
When Is Excisional Debridement Necessary for Chronic Wounds?
Table of Contents
ToggleQuick Summary:
- Used for Non-Healing Wounds – Recommended when a wound shows no improvement after 4 weeks and becomes clinically chronic.
- Removes Dead & Infected Tissue Quickly – Surgically eliminates necrotic tissue, slough, and eschar that block healing.
- Essential for Infection Control – Helps reduce bacterial load and prevents infections from spreading deeper into tissues.
- Breaks Down Biofilm Barriers – Physically removes biofilms that resist antibiotics and delay wound healing.
If you or someone you love is dealing with a wound that just won’t heal, you’ve probably heard the word “debridement” mentioned by your care team. In this blog, we’ll walk you through what this advanced surgical approach involves, how it differs from other wound care methods, the warning signs that indicate it may be necessary, and which patients are most likely to benefit from it. By the end, you’ll have a clear understanding of why this treatment can be a turning point for people struggling with chronic wounds.
What Is Excisional Debridement?
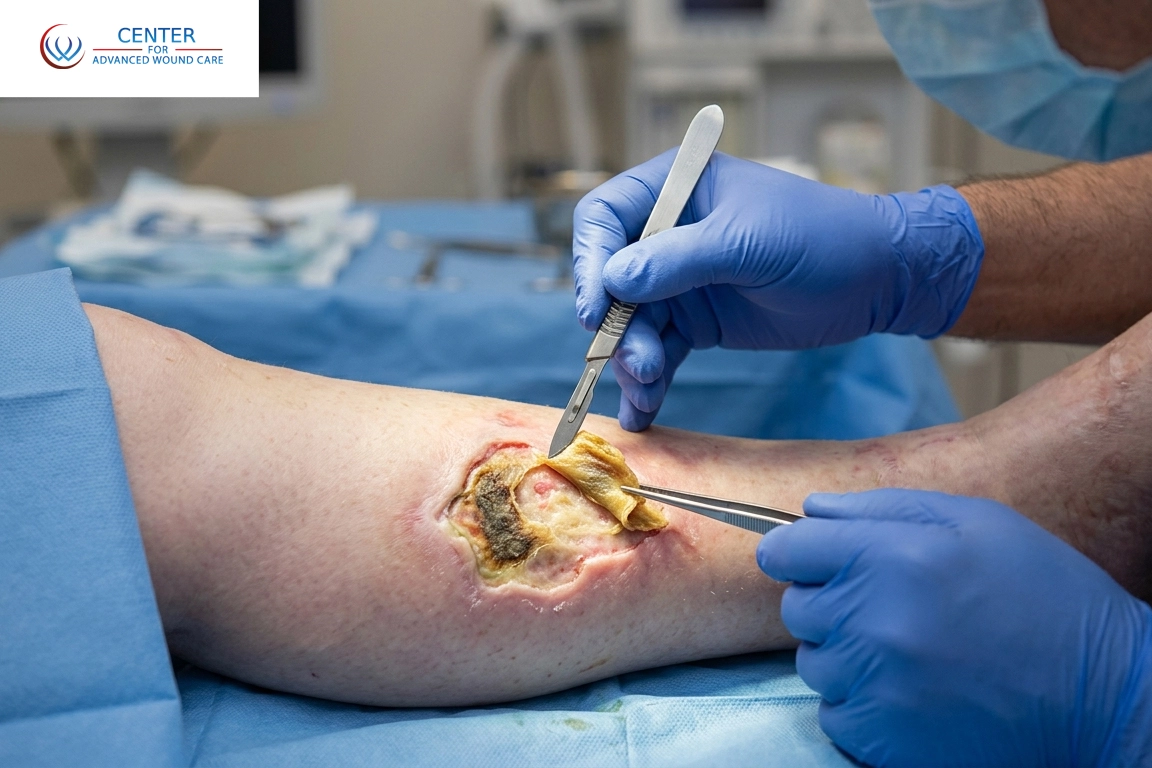
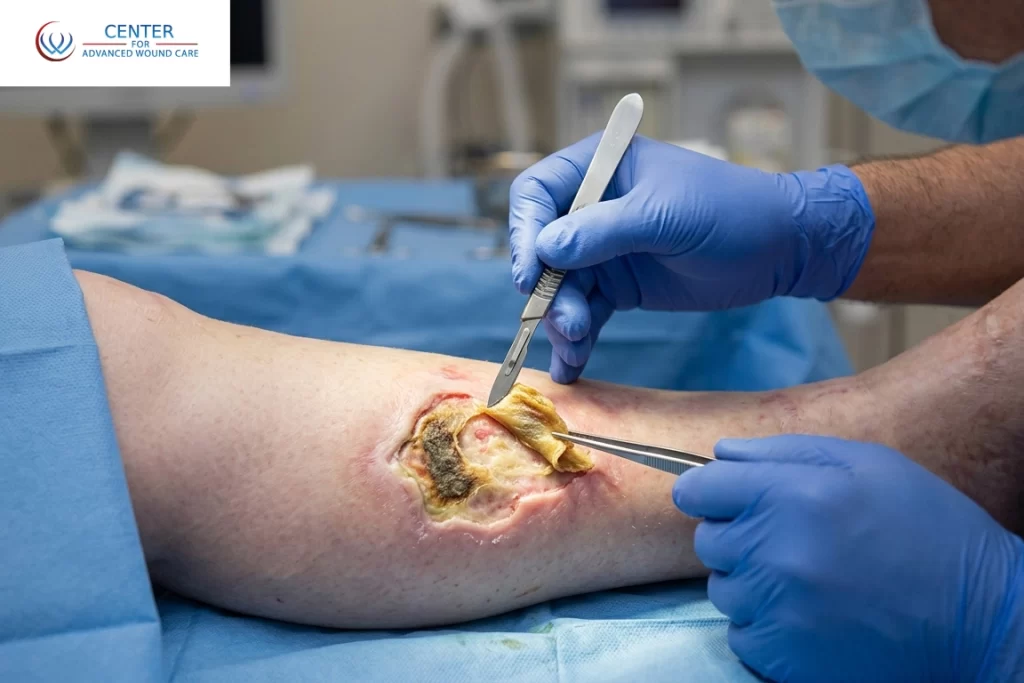
Let’s start with the basics. Debridement is the medical process of removing dead, damaged, or infected tissue from a wound so that healthy tissue can heal properly. There are several methods available, including topical treatments and advanced dressings, but excisional debridement is the most direct and immediate approach.
In this method, a trained wound care specialist uses surgical tools such as a scalpel or scissors to precisely remove non-viable tissue. While it may sound intensive, it is often necessary when a wound has not improved for weeks or months.
Think of it like pruning a damaged branch from a tree, removing what is no longer viable allows healthy growth to resume.
How Is It Different From Other Types of Debridement?
You may have heard of other methods such as autolytic, enzymatic, or mechanical debridement. Each works differently:
- Autolytic debridement uses moisture-retaining dressings to allow the body to break down dead tissue naturally. It is gentle but slow.
- Enzymatic debridement uses topical agents to dissolve necrotic tissue. It is selective but may take weeks.
- Mechanical debridement physically removes tissue through irrigation or dressings, but it can affect healthy tissue as well.
Compared to these methods, excisional debridement for chronic wounds provides faster and more controlled removal of dead tissue. This makes it especially effective for wounds with thick eschar, heavy bacterial presence, or delayed healing.
Signs That Excisional Debridement May Be Necessary
Not every wound requires surgical intervention. Plenty of wounds respond well to conservative treatments like topical dressings, moisture management, and compression therapy. But there’s a point where a wound stops responding and that’s when your provider starts looking at more decisive options. Your care team may recommend excisional debridement when one or more of the following warning signs are present:
1. The Wound Has Not Healed After Four Weeks
A wound that remains open for more than four weeks is generally classified as a chronic wound. At this stage, the natural healing process is disrupted and often gets stuck in the inflammatory phase, preventing progression to tissue repair and regeneration. One of the main reasons for this delay is the presence of dead or damaged tissue, which acts as a physical barrier over the wound bed. This barrier blocks the growth and migration of new skin cells, making healing difficult despite proper wound care. Removing this tissue helps restart the healing process and allows the wound to move forward.
2. Presence of Eschar or Slough
Eschar and slough are common types of non-viable tissue found in chronic wounds, and both can significantly delay healing. Eschar appears as a thick, dark, leathery layer that covers the wound, while slough is softer, yellowish, or gray in appearance. Although they may seem protective, these tissues actually trap bacteria, reduce oxygen supply, and prevent proper assessment of the wound’s depth and severity. If left untreated, they can worsen the wound condition. Removing them is essential to expose healthy tissue and create an environment where healing can begin.
3. Signs of Infection
Infection is a major factor that prevents wounds from healing effectively. Common signs include foul odor, increased or discolored drainage, redness around the wound, swelling, and warmth in the surrounding skin. In more severe cases, the infection may spread to nearby tissues or deeper structures. Dead or infected tissue provides an ideal environment for bacteria to grow, making it difficult for antibiotics or topical treatments to work effectively. Removing this compromised tissue helps reduce bacterial load, control the infection, and support faster recovery.
4. Biofilm Formation
Biofilms are structured communities of bacteria that attach to the wound surface and produce a protective layer around themselves. This layer acts as a shield, making the bacteria highly resistant to antibiotics and the body’s immune response. Biofilms are a common reason why chronic wounds fail to respond to standard treatments. They maintain a constant state of inflammation, preventing the wound from progressing through normal healing stages. Physical removal of the affected tissue is often necessary to break down this barrier and allow effective treatment.
5. Worsening Wound Structure
When a wound starts to worsen instead of improving, it is a clear sign that more advanced care is needed. This may include increased depth, widening of the wound, tunneling beneath the skin, or undermining where the tissue breaks down under the edges. These changes indicate ongoing tissue damage and can make the wound more difficult to treat with basic methods. Direct intervention allows healthcare providers to remove damaged tissue, fully assess the extent of the wound, and apply appropriate treatment to prevent further complications.
Who Typically Needs This Treatment?
Excisional debridement for chronic wounds is commonly recommended for patients whose underlying health conditions interfere with the body’s natural healing process. These conditions often reduce blood flow, weaken the immune response, or increase the risk of infection—making advanced wound care essential.
1. People With Diabetic Foot Ulcers
Diabetic foot ulcers are among the most common reasons patients require advanced wound treatment. Diabetes can damage both blood vessels and nerves, a condition known as peripheral neuropathy. This makes it difficult for patients to feel pain or detect injuries early, allowing wounds to worsen unnoticed. At the same time, reduced blood circulation slows the delivery of oxygen and nutrients needed for healing. Removing dead or infected tissue helps reduce infection risk and significantly lowers the chances of complications such as amputation.
2. Patients With Venous Leg Ulcers
Venous leg ulcers develop due to poor blood circulation in the lower limbs, often caused by chronic venous insufficiency. When blood pools in the veins, it increases pressure and leads to fluid leakage into surrounding tissues. This creates a poor healing environment where wounds can persist for months. These ulcers frequently develop slough and biofilm, which delay recovery. Cleaning the wound bed allows compression therapy and advanced dressings to work more effectively, improving healing outcomes.
3. Individuals With Pressure Injuries
Pressure injuries, also known as bed sores, occur when prolonged pressure reduces blood flow to certain areas of the body. They are common in individuals with limited mobility, such as those who are bedridden or use wheelchairs. In advanced stages, these wounds can extend deep into muscle or bone and often contain necrotic tissue. Removing this damaged tissue is essential to prevent infection, promote healing, and avoid serious complications like sepsis.
4. Patients With Non-Healing Surgical or Traumatic Wounds
In some cases, wounds from surgery or injury fail to heal as expected. Factors such as infection, poor circulation, or underlying medical conditions can cause wounds to reopen or deteriorate over time. These non-healing wounds may develop dead tissue that blocks recovery. Removing this tissue helps restart the healing process and prepares the wound for closure, whether naturally or through additional medical procedures.
5. People With Necrotizing Soft Tissue Infections
Necrotizing soft tissue infections are rare but extremely serious conditions that spread rapidly and destroy healthy tissue. Often referred to as “flesh-eating” infections, they require immediate medical intervention. In these cases, removing infected and dead tissue is not just beneficial—it is life-saving. Prompt and aggressive treatment helps control the spread of infection and protects surrounding healthy structures.
Conclusion:
A wound that isn’t healing is sending a signal that something more is going on. Whether it’s compromised blood flow, infection, dead tissue blocking the healing process, or all of the above the right wound care team can identify the problem and offer solutions that actually work.
Excisional debridement is one of the most effective tools available for getting chronic wounds back on track. It’s not something to fear, it’s something that, when done at the right time by experienced hands, can genuinely change outcomes.
If you or someone in your care has a wound that’s been lingering, getting worse, or showing signs of infection, don’t wait. Contact us today to schedule a consultation with our wound care specialists and take the first step toward real healing.
Frequently Asked Questions
1. How do you know if a wound needs this procedure?
A wound may require this treatment if it fails to heal after several weeks, shows signs of infection, or contains dead tissue such as slough or eschar. Other warning signs include foul odor, increased drainage, redness, swelling, or worsening depth. When conservative treatments no longer improve the wound, healthcare providers may recommend this approach to remove non-viable tissue and support proper healing.
2. Is the procedure painful?
This treatment can cause some discomfort, but it is usually performed using local anesthesia or other pain management techniques to reduce pain during the process. After the procedure, patients may experience mild soreness or sensitivity around the wound area. Proper wound care and prescribed medications help manage post-treatment discomfort effectively and allow healing to continue smoothly.
3. How long does it take to heal after treatment?
Healing time varies depending on the size, depth, and severity of the wound, as well as the patient’s overall health condition. Some wounds begin to improve within a few weeks, while more complex cases may take several months. Consistent follow-up care, proper dressing changes, and management of underlying conditions like diabetes can significantly improve healing speed and outcomes.
4. How often is this treatment required?
The frequency depends on how the wound responds over time. Some individuals may need only one session, while others with chronic or severe wounds may require multiple treatments. Regular monitoring by a wound care specialist ensures that the wound remains clean and continues progressing toward recovery without complications.
5. Can chronic wounds heal without this procedure?
Some mild wounds may heal with conservative care such as dressings and medications. However, when dead or infected tissue is present, healing is often delayed or completely stopped. In such situations, removing the damaged tissue becomes necessary to allow new tissue to grow. Without proper intervention, the wound may worsen and lead to further complications.
6. What are the risks of this treatment?
Like any medical procedure, there are some risks involved, including bleeding, infection, or temporary discomfort. However, when performed by trained professionals, it is generally safe and effective. The benefits of removing damaged tissue and improving the healing process usually outweigh the risks, especially in cases where the wound is not responding to standard care.
7. Who typically needs this type of treatment?
This approach is commonly recommended for individuals with diabetic foot ulcers, pressure injuries, venous leg ulcers, or wounds that fail to heal after surgery or injury. People with poor circulation, weakened immune systems, or underlying health conditions are more likely to require this treatment to support proper healing.
8. What is the difference between this and other methods?
This method involves the use of surgical instruments to remove dead tissue quickly and precisely. Other approaches, such as enzymatic or autolytic methods, rely on slower natural or chemical processes. Surgical removal is often preferred for severe or infected wounds because it provides immediate results and allows better control over the treatment.
9. Does this treatment help prevent infection?
Yes, it plays an important role in infection control. By removing dead and infected tissue, it reduces the environment where bacteria can grow. This allows medications and the body’s natural defenses to work more effectively, helping the wound heal faster and lowering the risk of complications.
10. What happens if dead tissue is not removed from a wound?
If dead tissue remains in a wound, it can block healing and create an ideal environment for bacterial growth. This may lead to ongoing infection, increased inflammation, and worsening of the wound. Over time, untreated wounds can become deeper or more severe, potentially leading to serious complications such as tissue damage or even amputation in extreme cases.


